Yes, Blue Cross Blue Shield Cover Dental Surgery. Blue Cross Blue Shield provides coverage for dental surgery procedures.
Blue Cross Blue Shield is a well-known health insurance provider that offers comprehensive coverage for a wide range of medical services. When it comes to dental surgery, many individuals wonder if Blue Cross Blue Shield covers this type of procedure.
Dental surgery is a specialized branch of dentistry that involves various surgical procedures to treat oral health issues. It is an essential service for individuals who require extensive dental work such as tooth extraction, dental implant placement, or corrective jaw surgery. For those insured under Blue Cross Blue Shield, the good news is that dental surgery is typically covered by their insurance plans. This coverage ensures that individuals can get the necessary dental procedures they need without worrying about excessive out-of-pocket expenses. We will explore the coverage provided by Blue Cross Blue Shield for dental surgery and discuss important details that individuals should know.
Credit: www.forbes.com
Does Blue Cross Blue Shield Cover Dental Surgery?
Blue Cross Blue Shield provides coverage for dental surgery, ensuring that individuals have access to necessary procedures. The insurance company may cover either the entire cost or a portion of it, depending on the specific policy.
Are you wondering if Blue Cross Blue Shield covers dental surgery? We may discover the answer by delving into the specifics. Blue Cross Blue Shield provides various health insurance plans, but coverage for dental surgery may vary depending on the specific plan you have. It’s important to check your policy or contact Blue Cross Blue Shield directly to determine the coverage details.
When considering dental surgery, it’s essential to understand the potential cost involved. The cost of dental surgery can vary depending on factors such as the type of surgery, the complexity of the procedure, and the location. To get a more accurate estimate, you can consult with your dentist or oral surgeon, who can provide you with a treatment plan along with cost details.
- Factors Affecting Coverage for Dental Surgery
Several factors can affect the coverage for dental surgery under Blue Cross Blue Shield:
- Policy Type: Different Blue Cross Blue Shield plans offer varying levels of coverage for dental procedures.
- Pre-authorization: Some dental surgeries may require pre-authorization from Blue Cross Blue Shield before the procedure is performed.
- Medical Necessity: Blue Cross Blue Shield typically provides coverage for dental surgeries deemed medically necessary. This means that if the surgery is required for your overall health or to treat a specific condition, it is more likely to be covered.
- Out-of-Network Providers: Coverage may differ if you choose an out-of-network oral surgeon. It’s important to check whether your plan covers out-of-network providers and if any additional costs or limitations apply.
Keep in mind that this list is not exhaustive, and there may be other factors specific to your plan that can affect coverage for dental surgery. Be sure to review your policy documents or speak with a representative from Blue Cross Blue Shield to get accurate information about your coverage.
Overall, Blue Cross Blue Shield can provide coverage for dental surgery, but the extent of coverage will depend on your specific plan and the factors mentioned above. It’s always recommended to review your policy or contact Blue Cross Blue Shield directly for the most accurate information regarding dental surgery coverage.
Coverage For Dental Surgery Under Blue Cross Blue Shield
If you are a Blue Cross Blue Shield (BCBS) member and are wondering whether dental surgery is covered under your insurance plan, you’re in the right place. Dental surgery can be a major expense, and it is important to understand what types of procedures are covered, any limitations or exclusions, as well as any pre-authorization or referral requirements that may be necessary. In this article, we will address these key aspects of coverage for dental surgery under Blue Cross Blue Shield.
Types Of Dental Surgery Covered
BCBS offers coverage for a wide range of dental surgeries, ensuring that members can receive the necessary treatments without worrying about the financial burden. The specific procedures covered may vary depending on the specific BCBS plan you have, but commonly covered dental surgeries include:
- Extractions
- Root canal therapy
- Dental implant surgery
- Oral and maxillofacial surgery
- Periodontal surgery
These are just a few examples of the types of dental surgeries that may be covered by your BCBS plan. It is important to review your specific plan documents or consult with a BCBS representative to understand the exact coverage details.
Limitations And Exclusions
While BCBS generally provides coverage for dental surgery, there may be certain limitations and exclusions that you should be aware of. These limitations and exclusions may include:
- Cosmetic surgeries or procedures that are not medically necessary
- Experimental or investigational procedures
- Services provided by out-of-network providers
- Procedures not deemed medically necessary by your dental provider
It’s important to carefully review your BCBS plan documents to understand any additional limitations or exclusions specific to your coverage.
Pre-authorization And Referral Requirements
Some dental surgeries may require pre-authorization or referrals from your primary dentist or dental specialist. Pre-authorization is a process where BCBS reviews and approves the need for the surgery before it is performed. Referrals, on the other hand, may be needed when your primary dentist or dental specialist recommends a specific surgeon for the procedure.
It is crucial to familiarize yourself with any pre-authorization or referral requirements for dental surgery under your BCBS plan. Failing to fulfill these requirements may result in denial of coverage or additional out-of-pocket expenses.
In conclusion, Blue Cross Blue Shield offers coverage for a variety of dental surgeries. By understanding the types of dental surgery covered, any limitations or exclusions, as well as pre-authorization and referral requirements, you can confidently navigate the process of obtaining the necessary dental surgery while maximizing your insurance benefits.

Credit: Youtube
Determining The Cost Of Dental Surgery
When it comes to dental surgery, one of the concerns patients often have is the cost. The cost of dental surgery can vary depending on various factors such as the type of procedure, the provider you choose, and your insurance coverage. Understanding these factors can help you determine the potential out-of-pocket costs and make informed decisions.
Out-of-pocket Costs
Out-of-pocket costs refer to the expenses you are responsible for paying directly, without insurance coverage. For dental surgery, these costs can include:
- Surgeon’s fees
- Anesthesia fees
- Pre-surgery consultations and examinations
- Post-surgery medications and follow-up appointments
It’s important to note that these costs can vary depending on the complexity of the procedure and the specific requirements of your case. Before undergoing dental surgery, it is recommended to ask your provider for a detailed breakdown of the potential out-of-pocket costs you may incur.
Deductibles And Coinsurance
Deductibles and coinsurance are terms commonly associated with insurance plans, including dental coverage. Here’s what you need to know:
- Deductibles: Before your insurance starts paying for anything, you have to pay a certain amount, called a deductible. For dental surgery, this could be a specific amount or a percentage of the procedure’s cost.
- Coinsurance: Once you have met your deductible, coinsurance is the percentage of the total cost that you are responsible for paying. For example, if your insurance covers 80% of the dental surgery cost and you have a 20% coinsurance, you would need to pay the remaining 20% as your share.
It is crucial to review your insurance plan’s terms and conditions regarding deductibles and coinsurance for dental surgery. Understanding these factors can help you estimate your portion of the cost accurately.
In-network Vs. Out-of-network Providers
Another factor to consider when determining the cost of dental surgery is whether your chosen provider is in-network or out-of-network. Here’s what you need to know:
- In-Network Providers: In-network providers have negotiated contracts with your insurance company, resulting in discounted rates. Choosing an in-network provider can help lower your out-of-pocket costs.
- Out-of-Network Providers: Out-of-network providers do not have contracts with your insurance company, which means you may have higher out-of-pocket costs if you choose to receive care from them.
It’s essential to check your insurance plan’s network and see if your preferred provider is included. This step can help you determine the potential cost difference between in-network and out-of-network providers.
By considering these factors – out-of-pocket costs, deductibles and coinsurance, as well as in-network vs. out-of-network providers – you can gain a better understanding of how your Blue Cross Blue Shield insurance coverage may affect the cost of dental surgery.
Factors Affecting Coverage For Dental Surgery
Factors that can affect coverage for dental surgery by Blue Cross Blue Shield include the specific dental plan, the severity and necessity of the surgery, and any pre-existing conditions or limitations outlined in the policy. It is important to review the policy and consult with the insurance provider to determine the extent of coverage for dental surgery.
When it comes to dental surgery, understanding your insurance coverage is crucial. Blue Cross Blue Shield offers various policy types and coverage levels that can affect your dental surgery coverage. Additionally, factors such as medical necessity, pre-existing conditions, and waiting periods play a significant role in determining the extent of coverage you may receive. Let’s explore these factors in more detail:
Policy Type And Coverage Level
The policy type and coverage level you have with Blue Cross Blue Shield can directly impact the coverage for dental surgery. Depending on your plan, you may have different levels of coverage, such as basic or comprehensive. It’s essential to review your policy documents or contact Blue Cross Blue Shield directly to understand the specific coverage details of your plan.
Medical Necessity
Medical necessity is another crucial factor affecting coverage for dental surgery. Blue Cross Blue Shield typically covers dental surgery procedures that are deemed medically necessary. These may include oral surgery for impacted wisdom teeth, jaw surgery for misalignment, or reconstructive surgery due to trauma or disease.
Pre-existing Conditions And Waiting Periods
Pre-existing conditions and waiting periods can also impact coverage for dental surgery with Blue Cross Blue Shield. Prior to coverage for certain treatments, some plans may impose waiting periods. It’s essential to review your policy details to understand if there are any waiting periods or limitations related to pre-existing conditions.
In conclusion, several factors can affect the coverage for dental surgery with Blue Cross Blue Shield. These include the policy type and coverage level, medical necessity, and the presence of pre-existing conditions or waiting periods. To ensure you have a clear understanding of your coverage, it’s advisable to review your policy documents or reach out to Blue Cross Blue Shield directly.
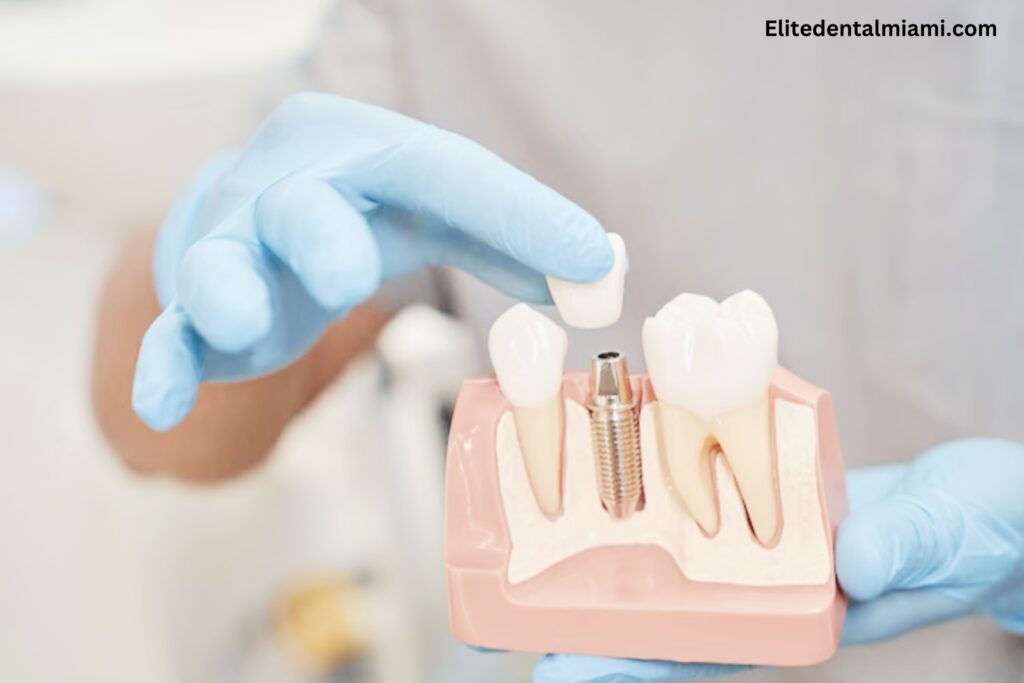
FAqs Of Does Blue Cross Blue Shield Cover Dental Surgery
What Does Medicaid Cover For Dental For Adults In Texas?
Medicaid in Texas covers dental services for adults without any out-of-pocket expenses. However, members in the CHIP program may have to pay a copayment for certain non-preventive services. Preventive services like exams, x-rays, cleanings, and sealants are not subject to copayments.
How Much Is Dental Insurance In Texas?
The cost of dental insurance in Texas varies. Dental insurance options that are cheap are available.
Does Fedvip Cover Braces?
Yes, Fedvip dental plans cover braces, but there may be a waiting period before you can receive this benefit.
Does Blue Cross Blue Shield Cover Dental Surgery?
Yes, Blue Cross Blue Shield provides coverage for dental surgery. Coverage amounts, however, could differ from one plan to the next. It is recommended to check with your insurance provider for details on coverage, including deductibles, copayments, and any pre-authorization requirements.
Conclusion
To answer the question, Blue Cross Blue Shield does provide coverage for dental surgery. Whether the insurance company covers the entire cost or only a portion of it depends on the specific policy. It is important to review the details of your plan and consult with your insurance provider to understand what is covered and any potential out-of-pocket expenses.
Remember to check with your dentist and ensure they are in-network with your insurance plan to maximize your coverage. Taking these steps will help you make informed decisions about your dental surgery and ensure you utilize your insurance benefits effectively.

I am a dentist and also blog regularly. my target audience is America Europe & providing regular information for them.
1 thought on “Does Blue Cross Blue Shield Cover Dental Surgery Implants?”